What is instability?
The shoulder joint is a ball and shallow socket joint. Under normal circumstances the ball is sat centrally on the socket, a bit like a golf ball sitting on a golf tee. When the shoulder joint becomes unstable the ball has a tendency to slide off the socket, most commonly to the front, however, this can be backwards, or downwards. The shoulder is the most flexible joint in the human body. This flexibility comes at the expense of stability and as a result, the shoulder joint is the most commonly dislocated joint in the body.
What causes shoulder instability?
The stability of the shoulder is dependent upon four things:
- The shape of the ball and socket joint
- The lining of the socket
- Ligaments connecting the ball to the socket
- Muscles surrounding the joint.
Either damage to or abnormalities of, one or more of these structures may compromise the stability of the shoulder joint.
Current thinking describes shoulder instability of three varieties:
- Shoulder dislocations most commonly occur as a result of a traumatic event. A great deal of force is required to dislocate the shoulder, and often the shoulder has to be put back into joint (reduced) in hospital under sedation. As a result of the dislocation there may be tearing of the lining of the socket, ligaments or tendons of the shoulder and/or fractures of the bones.
- Some individuals are inherently more flexible than others, sometimes referred to as being “double jointed”. These people can develop instability of the shoulder without precipitating trauma or only a minor event.
- A third type of instability, termed “muscle patterning” exists. In these cases instability of the shoulder joint is caused by a lack of muscle coordination as the shoulder joint moves. Certain muscles may be working too hard, or muscles may be activated in the wrong order.
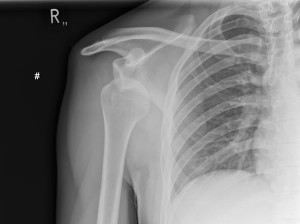
Will I need any further investigations?
X-rays of the shoulder are helpful as these can sometimes show signs of damage that has occurred as the shoulder dislocated. More detailed tests such as, CT or MRI scans may also be required. MRI scans are performed to show the extent of soft tissue (labral) damage and help with surgical planning. A dye may be injected into the joint (arthrogram) prior to the MRI scan to more accurately visualise and locate the tear. A CT scan is a better test to look at the bone structure of the joint in more detail and might be needed if there is a concern that there is significant underlying bone damage.
What problems does shoulder instability cause?
Recurrent dislocation
Some people may sustain a traumatic dislocation to their shoulder and, after it has been reduced, the shoulder joint goes on to function normally and does not give rise to further episodes of instability. Certain groups of patients, however, are at an increased risk of further dislocations or symptomatic instability after a first traumatic dislocation. It is well established that male gender, age less than 25, participation in contact sports such as rugby and bone damage all increase the risk of recurrent instability and dislocations.
Symptomatic instability without dislocation
Even if a shoulder does not come fully “out of joint”, it may be unstable to the extent that certain movements of the shoulder are difficult due to a sensation of impending dislocation (apprehension). This often accompanied by pain and a feeling of weakness.
Wear and tear (arthritis)
It is likely that patients who have had shoulder dislocations have an increased risk of developing shoulder arthritis later in life. It is logical that the greater the number and frequency of dislocations, the greater the damage is done to the joint surface and the greater the risk of arthritis. Similarly, if a shoulder can be prevented from having on going episodes of instability, it seems logical that the damage will be less. Having said this, no scientific study has demonstrated that treatment of instability reduces the incidence of arthritis.
What can be done to treat shoulder instability?
As mentioned above, shoulder instability is very complex and can be due to more than one cause, or a combination of causes. There is no treatment for shoulder instability that is 100% effective in every case. Your surgeon will help you decide which treatment is likely to be most effective.
Treatments can be divided into those involving surgery and those not involving surgery:
Non-surgical treatment:
Physiotherapy
Irrespective of the cause of shoulder instability, physiotherapy is a vital component of treatment. In cases of atraumatic and muscle patterning instability, physiotherapy is effective in strengthening and coordinating groups of muscles to work effectively and thus reducing episodes of instability. Many cases of traumatic instability are also effectively treated with physiotherapy.
Surgical treatment
In cases of traumatic instability where there is a high risk of further episodes or when a patient has suffered repeated dislocations surgery may be effective in improving symptoms. Through a series of small keyholes, arthroscopic surgery allows the repair of torn ligaments deep inside the shoulder joint. Small plastic plugs attached to sutures are inserted into the bone. The sutures can be passed through the ligaments to reattach them to the bone. Although relatively rare, sometimes the damage to the bones of the shoulder joint is so severe that keyhole ligament repair is not appropriate. In these instances a piece of bone from the shoulder blade is moved to the front of the shoulder socket, making it wider and therefore more difficult for the shoulder to dislocate (Latarjet procedure). This is most commonly performed through a more traditional open incision, rather than a keyhole.
Patients with atraumatic or muscle patterning instability do not generally respond well to surgery. In rare cases keyhole surgery can be used to tighten the shoulder joint lining. The effects of this are temporary and only when combined with intensive physiotherapy can this procedure durably improve symptoms
What is the success of surgery?
Generally, arthroscopic stabilisation surgery is a safe and reliable operation to make the shoulder feel secure and reduce the chance of the shoulder dislocating again. There is however a reported 10% risk that a further dislocation episode occurs.
What are the potential risks of surgery?
Any surgical procedure carries risks, however every effort is made to minimise these to ensure the best possible outcome from your surgery. The risks of the operation include infection, bleeding and nerve damage. There is also the possibility of further instability if the rehab regime from the physiotherapist is not followed properly and people return to activity too quickly. The shoulder can occasionally get stiff after surgery but this will usually loosen with physiotherapy and time. The Latarjet procedure is a more complex operation and has added risks including failure of the bone to heal to the glenoid (shoulder socket).
What is the recovery after surgery?
The shoulder will be protected in a sling after the operation for a period of 4 weeks. During this time you begin a supervised rehabilitation programme under the guidance of a physiotherapist. Physiotherapy is essential after the operation, to encourage good movement, rehabilitate the muscles back to normal function and ensure you are making good progress. You will see a therapist prior to discharge from the hospital. You will be given painkillers to take home after surgery. The use of an ice pack on the shoulder may also be helpful for the first few days after surgery. You will be seen in clinic two weeks after surgery to check the wounds and assess your progress. There are no sutures to be removed.
When can I return to normal activities?
Return to work depends on the nature of the job and your speed of recovery. You can return to desk and computer work when you feel comfortable to do so. You will be unable to drive for 4 weeks until after the sling is removed. The timescale for which you can go back to any previous sport or activity will depend on your movement and strength and the particular activity you have in mind. Examples include cycling 10 to 12 weeks, gentle swimming 10 to 12 weeks, light racket sports using operated arm 12-16 weeks, contact sports four to six months.
